Pain is the most frequently cited reason for a physician’s consultation across the United States. One in three Americans suffers from chronic pain every year. The most common reason for not working or missing school days is musculoskeletal discomfort. The currently accepted treatments include non-steroidal anti-inflammatory medications, including steroid injections and surgeries, and painkillers derived from opiates, each with a distinct risk profile. The most needed are effective, safe, low-risk treatment options for pain. Since the beginning of time, low-level treatment with laser (light) therapy (LLLT) and LED therapy (also called photobiomodulation) has been proven to reduce edema and inflammation-inducing analgesia, as well as aid in healing for a variety of musculoskeletal diseases. This paper aims to discuss the benefits of LLLT in treating pain and inflammation, the biochemical mechanisms behind its action, the dose-response curves, and how orthopedic surgeons could use LLLT to improve outcomes and decrease adverse effects.
With the anticipated chronic pain epidemic in developed nations, it is essential to establish cost-effective and secure methods of managing pain that will allow people to lead healthy and productive lives. In addition, including LLLT (utilized by numerous disciplines worldwide) in the American health care professional’s arsenal would provide new treatment options for patients. A unique and cost-effective method of treating pain may improve quality of life and reduce costs.
Keywords muscles; pain Laser therapy at low levels Photobiomodulation, Injury Repair
Abbreviations
LED: Light Emitting Diodes; LLLT: Low Level Laser Therapy; PBM: Photobiomodulation; NO: Nitric Oxide; ATP: Adenosine Triphosphate; ROS: Reactive Oxygen Species; MMP: Membrane Potential
Introduction
Musculoskeletal discomfort affects more than 116 million Americans yearly, with an estimated expense of $635 billion yearly in medical costs, loss of productivity, and missed working or going to school1. Each treatment has its advantages but has diverse side effects, risks, and complications. The current treatment options for muscular and skeletal pain involve immobilization, medication and chiropractic treatment, physical therapy, psychological management, injections, and surgical procedures. The standard treatments have particular risks and associated side effect profiles, which include gastric bleeding and peptic ulcers, systemic effects (cardiovascular) [4infection (including the epidural abscess) [56), deformities, neurological impairments, and surgical complications. The typical course of chronic pain is growing impairment, dysfunction, and disability.
The definition of the word “pain” used by The “International Association for the Study of Pain” states that “Pain is an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage [8]”. The withdrawal of the stimulus is usually a quick resolution of pain. However, pain sometimes persists even after removing the incentive or after the body has healed. It can also occur even without incident, injury, or disease. Acute pain lasts for less than 30 days.
In contrast, chronic pain can be described as having longer than six months or “pain that extends beyond the expected period of healing.” There are three kinds of pain: nociceptive central and neuropathic. The current treatment for analgesics or pain relief at different stages of channels of pain (Figure 1.). Clinically, low-level laser therapy (LLLT) can help treat nociceptive [9] as well as nerve pain [10], whereas central pain has not been proven to respond to LLLT.
What is LLLT?
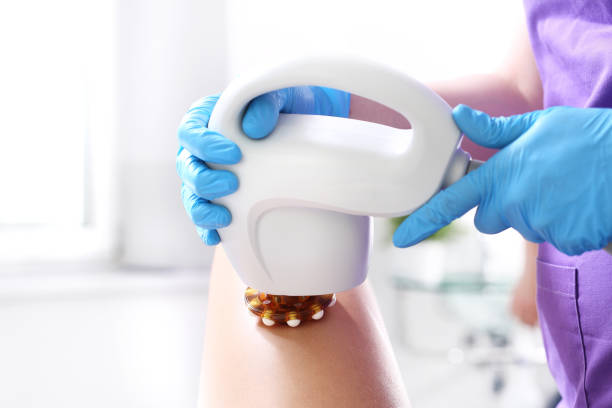
Low-Level Laser Therapy (LLLT), often referred to as Low-Level Light Therapy or Photobiomodulation (PBM), is the use of Low-intensity treatment using light. The effects are photochemical, not thermal. The light causes biochemical changes within cells. This could be compared with photosynthetic processes within plants. The photons are absorbed by the photoreceptors of cells and trigger chemical changes.
History of LLLT
In 1903 the doctor In 1903, Dr. Nils Finsen was awarded a Nobel Prize for his contribution to the treatment of various diseases, including lupus vulgaris, by concentrating light radiation [1111]. In 1960, Prof. Maiman Th [12] constructed the first operational Red ruby laser. However, it wasn’t until 1967 that Mester E et al. [13,14] could demonstrate the concept that is known as “laser bio stimulation” [13,14[13,14]. In 1999, Whelan H et al. [15] presented their research on the medical uses of lighting-emitting diodes (LED) in NASA’s space station. NASA satellite [1515. Then, over 400 Phase III randomized, double-masked trial designs that are placebo-controlled have been published, including more than 4000 lab studies on LLLT. (Pubmed.gov)
A laser is a machine that produces light via an optical amplification process by stimulating the emission of electromagnetic energy. There are four primary categories of lasers as defined according to the International Engineering Consortium (IEC standard 60825.) These classifications indicate a risk the radiation poses to the eyes.
-
- Class 1/1M-CD player
- Class 2/2M- laser pointer
- Class 3R/3B LT and DVD and CD writers
- Class 4 Laser Surgical
LLLT is the use of light (usually the low-powered laser or LED ) with a typical power is (10mW-500mW). Light with wavelengths in the red-to-near-infrared area of the spectrum (660nm-905nm) is commonly employed due to the capability of piercing skin and soft/hard tissues (Figure 2.). It has been proven by clinical trials to have a practical impact on inflammation pain and tissue healing. Its power density (irradiance) is typically between 5W/cm2 that is used to treat an injured area or the site of discomfort for 30-60 seconds several times per week for many weeks. The result is decreased pain, inflammation, and an acceleration of tissue regeneration. Most of the time, the LEDs or lasers used in LLLT emit divergent beams (not collimated or focused) since collimation is not removed from the tissue, and because of this, ocular risks are decreased over distance.